Periodontics (gum disease)
Caring for and treating the gums and other supportive structures.

Periodontics is a special brand of dentistry that focuses on the gums and other dental supportive structures, including your jaw bone. The gums are incredibly important when it comes to dental health, and if there’s an issue with your gums, it can even threaten the health of your teeth.
Whenever you visit your dentist for a check-up, they will inspect your gums just as much as they look at your teeth. If they spot any issues, they will let you know if it’s something you can take care of at home with good hygiene, something they can help with in the dental practice or something that you will need to see a dedicated periodontist to treat.
Whatever the case, periodontics can help to keep your oral health in good shape and avoid problems before they arise.
What is periodontics?
Periodontics is a specialist type of dentistry. It looks specifically at the gums and even the jawbone in relation to how these structures support the teeth.
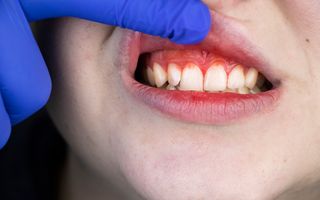
One of the most common problems that periodontics deals with is gingivitis and gum disease, which occur in the gums, they are quite common but can be very damaging for your teeth if left untreated.
However, periodontics also deals with:
- Placing dental implants
- Scaling and tooth root cleaning (root debridement)
- Gum lifts and other cosmetic gum surgeries
- Bone and gum grafting
- Crown lengthening
- Periodontal surgery
As our gums help to nurture and support our teeth, they’re very important for our overall dental health. So when you look after your gums, you’re really looking after your teeth and helping to maintain a bright, healthy smile.
What does a Periodontist do?
All qualified dentists have a good general understanding of periodontics and can perform basic periodontal treatments.
A Periodontist, however, is a specialist in this field. They are usually required for more intensive procedures, such as bone and gum grafting, periodontal surgery, and placing dental implants. You will also likely see your Periodontist regularly if you are recovering from any of these procedures.
To see a Periodontist, you will usually visit your general dentist, then they will refer you to a Periodontist should your treatment require specialist attention. In some cases, there may be a Periodontist working in your usual dentistry practice, but you may have to go to a different practice if not.
What are the advantages of receiving periodontics?
Periodontal treatment is a must for anyone with issues with their gums. Here are the key benefits.
- Avoid further issues: Periodontal treatment such as cleaning and scaling can help to keep gingivitis at bay, which can prevent the condition from worsening into periodontitis (which is a lifetime condition once you have it).
- Protect your teeth by caring for your gums: Healthy gums support healthy teeth, meaning that caring for this support system is a great way to keep your teeth in good shape.
- Treat periodontitis: Periodontitis can be a serious condition that leads to the loss of teeth. With treatment, you can manage this condition and prevent losing teeth or damaging the bone.
What to expect from your periodontal appointment
The exact details of your periodontal appointment will vary depending on whether you’re visiting for a check-up and clean or if you’re getting treatment.
Here’s what to expect from a standard check-up and clean with a Periodontist:
- Brush and floss your teeth before you arrive
- Your Periodontist will ask about any symptoms you’ve had, such as swollen, red, or bleeding gums
- They will do an oral exam and check for plaque
- If you already have gum pockets, they will take note of the size of these pockets
- Your dental professional will take x-rays to check for bone health below the gums
- Based on your oral health, your Periodontist will recommend a treatment plan, including changes you can make at home
If you suffer from gingivitis and want to reduce your infector, or you have periodontitis and you want to ensure you can manage your symptoms, you should consider speaking to a qualified Periodontist. By speaking to a periodontist early, you can significantly improve and manage your oral health.
Get in touch with our friendly team to schedule an appointment.
Frequently asked questions
Periodontitis is the advanced form of gingivitis, a disease where your gums become infected. Gingivitis and periodontitis come from poor oral health, such as not brushing and flossing well or often enough, and consuming a diet high in sugary foods and drinks.
While gingivitis can be reversed with good oral health and a professional clean from your dental hygienist, periodontitis cannot be reversed. Once the disease has reached this stage, it becomes about managing the symptoms and stopping it from getting worse.
Unfortunately, there is no treatment or medication that can ‘heal’ periodontal disease. Once you have it, your periodontist will help you to manage the symptoms through measures such as regular cleanings and flap surgery.
The best treatment for gum infection is good oral hygiene at home, including brushing and flossing, and avoiding a diet high in sugary foods and drinks. It is also important to visit your dentist for a professional cleaning and further treatment options if needed.
A Periodontist is a specialist kind of dentist who focuses solely on the periodontal area of the mouth - the gums and jawbone beneath the gums. They perform a variety of treatments, from simple procedures such as removing plaque from teeth to implanting false teeth and doing gum grafts.
Their job is to ensure your gums are healthy and well enough to support your teeth and, therefore, your oral health overall.

